New training model mimics real-world surgery for WVU residents
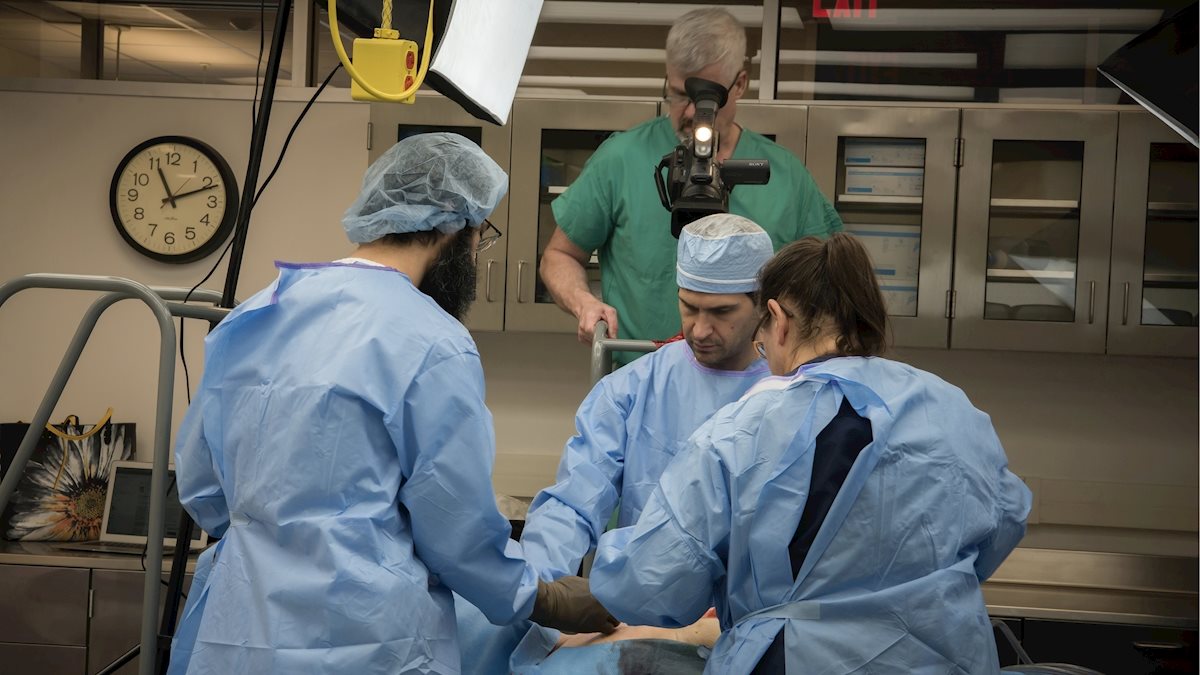
Instinct— surgeons act on it in the operating room, but it can be difficult-- though not impossible-- to teach, thanks to a perfused cadaver training model at the West Virginia University School of Medicine that mimics real-world surgery conditions.
Surgical residents are placed in simulated operating rooms, working with fresh cadavers which are connected to perfusion machines that pump simulated blood through the body. This allows the blood vessels and tissues to “bleed” as they would in live patients.
The surgeons can then treat the “patient” as if they were treating a real injury – exposing and controlling blood vessels-- ultimately stopping the “bleed.”
“It’s as close as we’ve come to mimicking the effects and intensity of the operating room,” Daniel Grabo, M.D., director of trauma education at WVU, said. “When you have moments to react, you draw on your experience. Today, the majority of routine surgeries are done with less invasive procedures which create gaps in hands-on training and experience for emergencies and critical injuries.”
The residents use the perfused cadaver model to train in trauma, open vascular, thoracic and advanced liver and biliary procedures. In some cases, the training provides immediate results, as was the case for Patrick Bonasso, M.D., WVU surgery resident.
Dr. Bonasso completed a simulated operation using the perfused cadaver model the same day he performed the procedure on an admitted patient.
“Surgery is about repetition and being comfortable in your skillset. You have a split-second to manage bleeding and perform care,” Bonasso said. “I was better prepared to treat my patient because I had walked through this same scenario just hours before I was in the actual operating room.”
The Fresh Tissue Training Program, which houses the perfused cadaver model, is a collaborative effort between WVU’s Critical Care and Trauma Institute and the Departments of Pathology and Surgery. Faculty from these disciplines identify emerging trends from the Accreditation Council for Graduate Medical Education and then look at the number of surgical cases residents perform at WVU. Based on that data, they identify any potential deficiencies in surgical opportunities and mediate that with the perfused cadaver training.
“Unfortunately, it’s difficult to develop these skills only at a patient’s bedside these days,” Grabo said. “You need to be able to act in the moment – and it’s not just something we can create for our residents.”
To learn more about surgery education at WVU, visit medicine.hsc.wvu.edu/surgery.
-WVU-
cat 11/16/18
CONTACT: Cassie Thomas
WVU School of Medicine
304.293.3412; cassie.thomas@hsc.wvu.edu