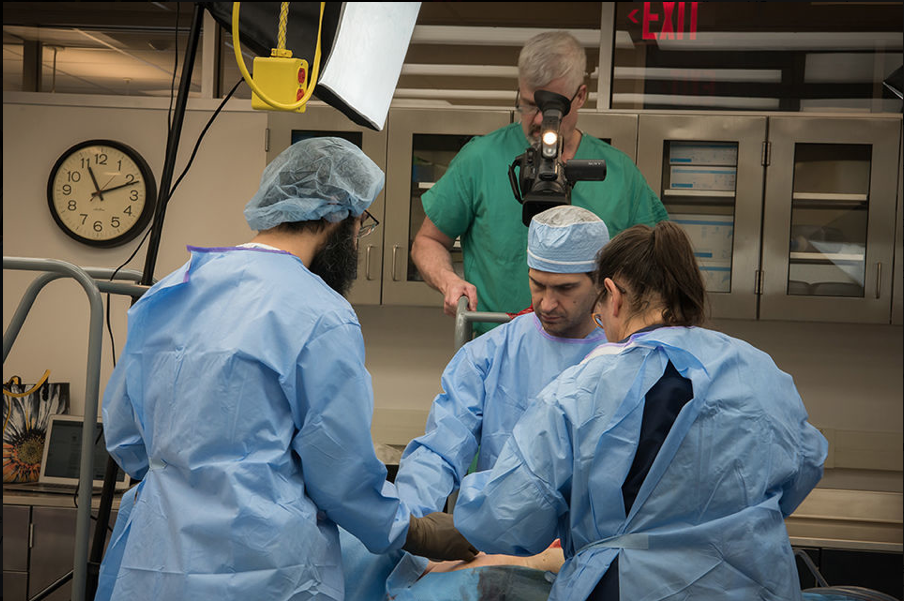
Fresh Tissue Training Program
We are very excited about our Fresh Tissue Training Program. At the beginning of the academic year, our trauma team works on many trauma procedures, including peripheral vascular injury, IVC injury, thoracotomy, and cardiac injury. In the spring our general surgery teams work through foregut, thoracic and open general surgery including hepatectomy, vagotomy, and antrectomy, and open common bile duct exploration.
We are fortunate to be able to use of WVU Hospital's state of the art Autopsy Suite located at the Operational Support Center for our training. Check out these articles about the fresh tissue training program.
WV Executive
WVU Magazine
WVNews
OUR PARTNERS
Without our partners, the Fresh Tissue training Program would not succeed. We are deeply grateful for the support and enthusiasm we have received.
- Critical Care & Trauma Institute, WVH Medicine
- Department of Surgery, School of Medicine, WVU
- Department of Pathology Anatomy and Laboratory Medicine, School of Medicine, WVU
- Ruby Memorial Hospital Operating Room and Sterile Supplies, WVU Medicine
- Respiratory Care & Pulmonary Services, WVU Medicine
- The Human Gift Registry, School of Medicine, WVU
- Comprehensive Care Service, LLC
EDUCATIONAL PROGRAMS
- Advanced Surgical Skills for Exposure in Trauma (ASSET) Course
- Special Forces Medic Training Program
- Genearl Surgery Resident Training Program
RESEARCH
1. Grabo D, Bardes J, Sharon M, Borgstrom D. Initial Report on the Impact of a Perfused Fresh Cadaver Training Program in General Surgery Resident Trauma Education. American Journal of Surgery. 2020;220(1):109-113.
2. Grabo, D., Polk, T., Strumwasser, A., Inaba, K., Foran, C., Luther, C., Minneti, M., Kronsted, S., Wilson, A., & Demetriades, D. (2018). A novel, perfused-cadaver simulation model for tourniquet training in military medics. Journal of Special Operations Medicine, 18(4), 97-102.
3. Polk, T., Grabo, D., Minneti, M., Kearns, M., Inaba, K., Benjamin, E., & Demetriades, D. (2018). Initial report on a damage control surgery course for military forward surgical teams utilizing a novel perfused cadaver model for training and evaluation. Journal of the American College of Surgeons, 227(4-2), e40. doi: 10.1016/j.jamcollsurg.2018.08.106.
4. Leatherman, M. L. , Held, J. M. , Fluke, L. M. , McEvoy, C. S. , Inaba, K. , Grabo, D. , Martin, M. J. , Earley, A. S. , Ricca, R. L. & Polk, T. (2017). Relative device stability of anterior versus axillary needle decompression for tension pneumothorax during casualty movement. Journal of Trauma and Acute Care Surgery, 83(1), S136–S141. doi: 10.1097/TA.0000000000001488.
5. Linnebur, M. , Inaba, K. , Haltmeier, T. , Rasmussen, T. E. , Smith, J. , Mendelsberg, R. , Grabo, D. & Demetriades, D. (2016). Emergent non–image-guided resuscitative endovascular balloon occlusion of the aorta (REBOA) catheter placement. Journal of Trauma and Acute Care Surgery, 81(3), 453–457. doi: 10.1097/TA.0000000000001106.
6. Inaba, K. , Karamanos, E. , Skiada, D. , Grabo, D. , Hammer, P. , Martin, M. , Sullivan, M. , Eckstein, M. & Demetriades, D. (2015). Cadaveric comparison of the optimal site for needle decompression of tension pneumothorax by prehospital care providers. Journal of Trauma and Acute Care Surgery, 79(6), 1044–1048. doi: 10.1097/TA.0000000000000849.
7. Grabo, D. , Inaba, K. , Hammer, P. , Karamanos, E. , Skiada, D. , Martin, M. , Sullivan, M. & Demetriades, D. (2014). Optimal training for emergency needle thoracostomy placement by prehospital personnel. Journal of Trauma and Acute Care Surgery, 77(3), S109–S113. doi: 10.1097/TA.0000000000000349.